
The prognosis is usually poor and recurrence is frequent. The exact pathogenesis of LEC is still unclear, but its association with EBV in genetically predisposed populations suggests a role in carcinogenesis. The pathology is frequently described as a poorly differentiated carcinoma that consists of sheets of large atypical epithelial cells intermingled with benign inflammatory infiltrates rich in lymphocytes and plasma cells (lymphoid stroma) (Figure 1 & 2). 1, 3, 6, 8 LEC is, however, exceedingly rare in Caucasians of European ancestry and LEC in this population is often not associated with EBV.įor LEC in the head and neck, most patients develop an expanding painless mass with variable facial nerve involvement. Interestingly, LEC is the most common salivary gland malignancy amongst the Inuit population and represent over 90% of all cases. 7 Of the salivary gland cases, 80% are found in the parotid glands, 13% in the submandibular glands, and 5% in the minor glands. 2, 4 For the populations described, this malignancy is often found in the nasopharynx and major salivary glands and is strongly associated with Epstein-Barr virus (EBV). 1‒8 The mean onset is 40years old, and women are more frequently affected than men regardless of ethnicity. Lymphoepithelial carcinoma (LEC) is a rare malignancy that has a strong ethnic predisposition for Eskimos in the northern circumpolar region, Mongolians, and South-east Asians. It was emphasized that monitoring was not ideal as recurrence rate is very high and will drastically decrease survival however, the patient was lost to follow-up. The patient was given the option of close monitoring or a right parotidectomy and selective neck dissection followed by radiation therapy. The final pathology of the mass was lymphoepithelial carcinoma with an unknown primary: TxN1M0. Occult parotid malignancy with nodal involvement.Metastatic squamous cell carcinoma: micrometastatic disease.Multiple mucosal biopsies were taken during panendoscopy, and the frozen sections of these specimens were negative for malignancy. An excisional biopsy of the mass with panendoscopy was performed. PET/CT showed increased uptake in the right upper neck, but no evidence of disease elsewhere in the body.
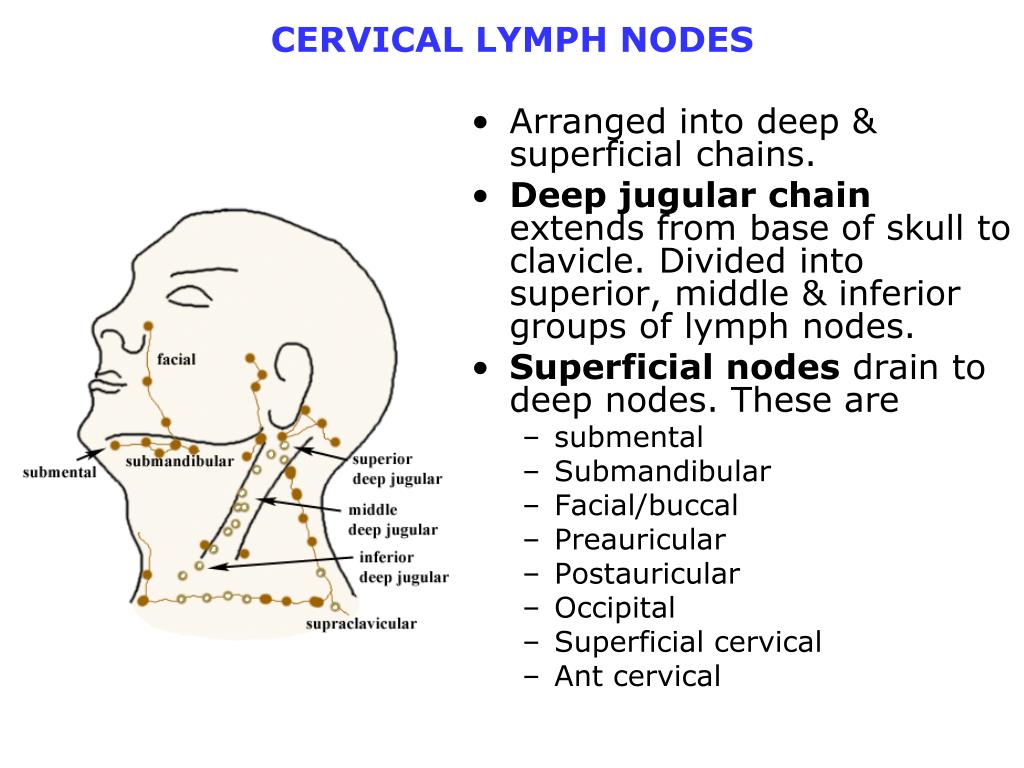
Ultrasonography of the mass revealed an ovoid solid structure measuring 1.5 x 0.9cm consistent with a lymph node with abnormal morphology. Other medical histories were non-contributory.ĬT with contrast was negative for parotid or submandibular enlargement bilaterally and there was no evidence of parotid or cervical lymphadenopathy elsewhere.
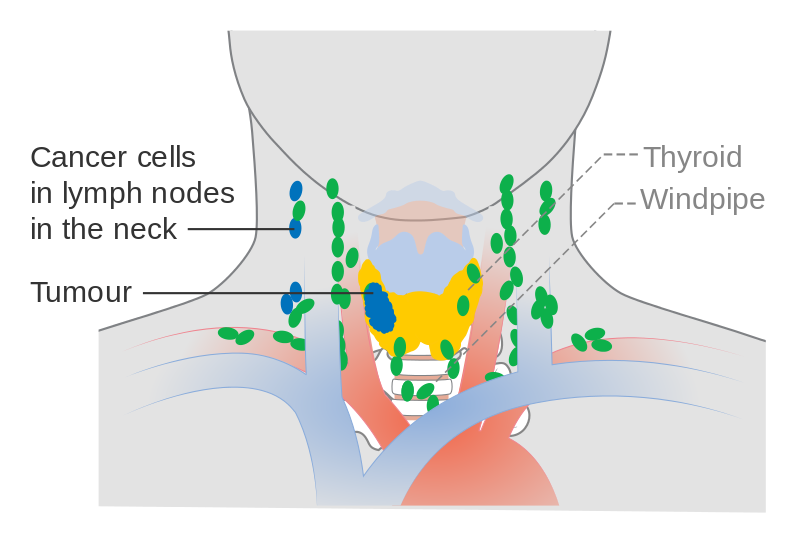
She has a history of squamous cell carcinoma of her lower eyelid that was removed via wide local excision with clear margins. The remainder of the exam was negative and exam with FFL was also negative for any masses or lesions. A complete head and neck exam was performed, and a 1x1cm rubbery, mobile nodule was palpated in the Level II nodal region. She denied any previous irradiation to her head and neck and she is a non-smoker with no history of alcohol abuse. She denied any unexplained weight loss, fevers/chills, otalgia, epistaxis, hoarseness, sore throat, odynophagia, or dysphagia. The patient did not recall details regarding the onset of the mass, but only that it has persisted for several months. The patient is a 74-year old white female who presented with a painless mass in the inferior margin of the right parotid gland.
